“Child is the father of the man.”
An adage that most of us would relate to. No doubt, children are the most important assets of any nation as they are of humanity. Moreover, even from a life perspective, childhood is one of the most critical stages of life that can have a long-term negative impact on the overall human life.
Undoubtedly, child (both infants and under 5-years) mortality rate is one of the most crucial socio-economic indicators for any nation, throwing light on the quality of life, especially from a general health and medical perspective. Thus, saving children and their right to live is one of the most important human considerations and it becomes imperative that there be a cohesive focus on the reduction of neonatal and child mortality rates.
A vice that grips many countries all over the globe – neonatal and child mortality is responsible for a major proportion (around 4 million) of all pediatric deaths. In fact, in India alone around 2.1mn. under-5 years children die each year with almost 50% of these deaths being within the first 28-days of their births. This alone accounts for one-third of the child and one-fourth of the neonatal deaths worldwide annually!
Given this scenario, it isn’t a surprise that over the last decade or so, there has been an increased and concerted thrust towards bringing this neonatal and child mortality rate down.
Neonatal & Child Mortality: The Determinants & Challenges
The child mortality rate, expressed per 1000 live-births, defines the probability of a child dying between the first and 5th year of life. Thus, it includes:
- Neonatal Mortality (first month)
- Post-neonatal Mortality (age 1–11 months)
- Infant Mortality (first year)
- Child Mortality (age 1–4 years)
This categorization brings into focus the other quintessential question on the determinants of child survival.
In India, the following factors determine the life expectancy and mortality rates of children falling under any one of the above stages:
- Maternal and demographic factors
Factors such as the age and education level of the expecting mother, the spacing between childbirths, maternal nutrition, and health awareness, and most importantly the availability and attendance of trained medical professionals at the time of delivery are important determinants of the survival rate of the newborn. Children born to illiterate mothers or females with less than 8-years of schooling, or those that are born to adolescent mothers, as well as those children who are born less than 2-years before the first birth, are at a higher risk compared to those born to educated mothers, at an appropriate child-bearing age with enough gap between two deliveries. Similarly, those children born to malnourished or obese mothers or those that are delivered at home by traditional attendants show a neonatal mortality rate of 27.2/1000 live births, in comparison to the mortality rate (25.2/1000 live births) in those born to healthy females attended by medical professionals at hospitals.
- Social and Economic Factors
The next set of factors that determine mortality are the socio-economic factors such as the social group the child is born in, economic status of the family, and of course the sex of the child. Research shows that children born in SC/ST/OBC families in India are at a 13% and 18% higher risk of dying in the neonatal and post-natal period, respectively. Surprisingly, the decline in the mortality rate among those born in low SLI (Standard of living Index) has considerably fallen compared to high SLI families that register no decline at all. Gender inequality and gender-discriminatory child rearing practices, too pave way for the growing IMR among girls with more girls dying than boys (IMR for boys being 39 and for girls 428)
- Environmental Factors
Finally, the environmental factors like good sanitation, access to clean drinking water, improved toilet facilities, etc. too, have their bearing on the mortality rates. The IMR and U-5 mortality rates are seen to be consistently lower among children born to or living in families who have access to these secure environmental factors as compared to those who accessed drinking water from unsafe sources or do not have access to an improved sanitation.
Challenges to better Newborn Survival and Child Health
Despite being a large country (and that too with the highest burden of neonatal and under-5 deaths), India has managed to make remarkable progress in registering a declined mortality rate compared with the global fall (over 50% in the last decade). Unfortunately, this decline has been an uphill task with the roadblocks and challenges that are rampant. Some of the challenges that India faces in ensuring better newborn survival and child health include:
- Undernutrition and malnutrition especially among adolescent girls and pregnant women.
- Social norms, socio-cultural factors and economic status that deter the accessibility of healthcare, nutrition, clean water and sanitation facilities in several regions or communities.
- Lack of accurate and comprehensive maternal, neonatal and child health information
- Illiteracy and low educational level of expecting mothers
- Non-availability of skilled personnel and specialists in child healthcare.
Neonatal & Child Mortality in India: The Fact Sheet
A forerunner in the global efforts to reduce neonatal & child mortality, India has exhibited continuous commitment towards this cause. The resultant 59% reduction in the under-5 and neonatal mortality rates since 1990 comes as no surprise. In fact, India has realized impressive improvement in child survival rates over the last two decades, with neonatal deaths falling from a staggering 1.3 mn. In 1990 to 875,000 in 2010, pegging the neonatal mortality at nearly 28% of the global neonatal deaths.
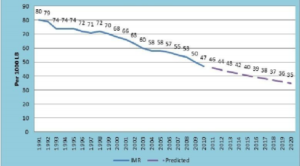
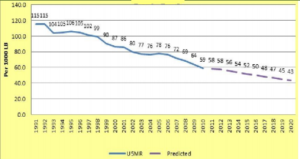
Historical & Predicted Trends of Infant and Under-5 Mortality Rates Respectively (1991-2020)
Source: National Institute of Medical Statistics
Yet, a lot remains to be done to reach the Millennium Development Goal of a two-thirds reduction in Under-5 mortality by 2020.
In India, since years there has been a marked evidence of the existence of child health inequalities along varied dimensions, presenting a unique context to the mortality case – from differentials across states to socio-economic disparities across issues like access to health facilities, health outcomes, and the insufficiency of the public health care systems in delivering equitable health services; to the closing gap of IMR between rural and urban areas.
While states like Tamil Nadu, Kerala, Maharashtra, Punjab, Himachal Pradesh and West Bengal have achieved the IMR and U-5 mortality rate goals, many other states remain far from achieving the targeted numbers. Further, even the early neonatal mortality rate continues to hover at 30/1000 live births, indicative of the poor quality of perinatal care available in the country.
Combating the Vices: What needs to be done?
In the Indian context, child survival emphasis requires strategizing by state and area to close the regional disparities in the health systems, develop community participation in child health and nutrition. A multi-sectoral approach, that includes the elimination of gender gap & early child-bearing, promotion of female education and nutrition, and an increased use of health services during pregnancy and delivery, is needed to achieve greater impact and accelerate the progress towards health goals.
Policies should be focused on addressing the causes of pediatric deaths such as preterm deliveries, sepsis, etc., through optimal coverage and easy access to specialized medical professionals, supplies and paraphernalia, institutional delivery facilities (like Emergency Obstetric Care facilities) for delivery, intrapartum, perinatal and neonatal intensive care. It is also important that there be an adequate focus on improving breastfeeding rates and on clean water, sanitation and hygiene practices even at household levels. Adequate attention to proper case management of diarrhea and pneumonia and inclusion of new vaccines to prevalent immunization programmes would also help substantially reduce child deaths in India.
Neonatal & Child Mortality: A Policy Perspective
Child survival (before and after birth and throughout childhood) and development (physical, mental, and social) has been at the core of all development plans in India and is recognized as an essential for the overall development of the society. Over the last few years, the Indian Government, exclusively as well as with support from regional and international bodies, including UNICEF, has continually focused on the improvement of maternal and child mortality rates, making a striking impact in these areas.
The Indian government, under its centrally-sponsored landmark programmes – Reproductive and Child Health Programme II, Integrated Child Development Services, NRHM (National Rural Health Mission), NHM (National Health Mission, and RMNCH+A Strategy (Reproductive, Maternal, Newborn, Child and Adolescent Strategy), has comprehensively integrated several interventions that aim at improving child survival, strengthening health systems and addressing factors that contribute to infant and under-5 mortality.
The above-mentioned schemes involve interventions such as the setting up of Special newborn care Units (SNCUs), Newborn Baby Corners (NBCCs), and Newborn Stabilization Units (NBSUs) for care of sick newborns, skills development among health personnel (Medical officers, Staff nurses and ANMs) for inpatient management of causative issues including poor birth weight and malnutrition in children, and home-based newborn care strategy to ensure the reach of quality antenatal care. Nutritional Rehabilitation Centres (NRC have also been built to treat severe and acute malnutrition cases in children through counseling of mothers and educating them on proper feeding techniques.
Besides these, several programmes such as the Janani Shishu Suraksha Karyakaram (JSSK) (2011), Navjaat Shishu Suraksha Karyakaram (NSSK) and Rashtriya Bal Swasthya Karyakaram (RBSK)(2013) too are being worked upon to counter the mortality concerns through the promotion of institutional deliveries by eliminating all out-of-pocket expenses for first 30-days from birth that deter expecting women and their families from seeking institutional healthcare; prevention of infections and initiation of breastfeeding; as well as provision of early and free diagnosis and management of defects at birth, diseases, deficiencies and developmental delays and disability.
Other noteworthy programmes include:
India Newborn Action Plan (INAP): Launched in 2014 in response to Global Newborn Action Plan, it lays out the roadmap to eliminate stillbirths and newborn deaths arising out of preventable causes. It uses high-impact and cost-effective interventions and a robust monitoring framework to achieve the goal of “Single Digit Neonatal Mortality Rate by 2030” and “Single Digit Stillbirth Rate by 2030”.
Pradhan Mantri Surakshit Matritva Yojna: Recognizing the intricate link between maternal health and child mortality, the GOI has recently launched this scheme that works towards ensuring a healthy pregnancy for the mother and a safe delivery to the child. Besides working at the grass-root levels to ensure the health and nutritional supplementation education, this scheme also provides for regular checkups for the mother to ascertain any health-related issues to both the fetus and the mother at the very onset for proper health and care management.
Project ĀSMĀN: International bodies like UNICEF too are leading the cause of Newborn and Child Health in India together with the government. They are not just actively involved in several of the above-mentioned initiatives, but also in Project ĀSMĀN launched in 2015 as one of the major healthcare initiatives aimed at reducing infant, neonatal and maternal mortality in India, through the facilitation of the availability of quality healthcare.
With such strong initiatives in place, it is only a matter of converting these commitments and resources into measurable results, especially among the children of the socially disadvantaged and marginalized communities.
India has witnessed a dramatic victory over the vices of neonatal and child mortality, reaching even the most hard-to-reach areas to ensure sound child health practices for the vulnerable children, despite several challenges. However, now the attention should be shifted towards tackling new-born mortality and stillbirths. India still records 0.76 million newborns deaths and a staggering 572,000 stillbirths each year. Child mortality improvement is not a far-fetched dream should adequate attention be given to contributing factors like disease-specific health interventions, alteration in nutrition and health behavior, and the availability of proper health care services.
Word count: 1919
Copyscape Results: No Private Index results found for the text you pasted (1,986 words), on 15 Mar 2017 at 12:07 GMT.
No Internet results found for the text you pasted (1,986 words), on 15 Mar 2017 at 12:21 GMT.
References
unicef.in/PressReleases/374/The-Infant-and-Child-Mortality-India-Report
http://unicef.in/Whatwedo/2/Neonatal-Health-
http://www.thelancet.com/pdfs/journals/lancet/PIIS0140-6736(10)61461-4.pdf
http://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.616.5553&rep=rep1&type=pdf
http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(10)61461-4/abstract?rss=yes
http://iegindia.org/upload/pdf/wp292.pdf
http://nipccd.nic.in/reports/imr.pdf
https://www.sjri.res.in/eppublicationdetail/909
http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0057244
http://bmcpregnancychildbirth.biomedcentral.com/articles/10.1186/1471-2393-14-357
http://www.isid.ac.in/~pu/conference/dec_12_conf/Papers/AnuRammohan.pdf
http://nrhm.gov.in/nrhm-components/rmnch-a/child-health-immunization/child-health/schemes.html
http://pib.nic.in/newsite/PrintRelease.aspx?relid=101932
https://www.newbornwhocc.org/INAP_Final.pdf